Tedi Asher, PEM’s resident neuroscientist, looks at play’s power to heal.
For millennia psychiatric disease has plagued the human population. It has remained difficult to treat, let alone to cure, in part because of its obscured etiology. We just didn’t understand enough about what goes on in the brain to generate these clusters of symptoms that we experience as mental illness. It was the introduction of technologies, like neuroimaging (e.g. fMRI), that allowed us to begin to identify biological markers of psychiatric disease; to point to a mark on a brain scan and say, “this is what’s wrong here.” It is these same neuroimaging technologies that are now enabling treatment of the disorders that they initially delineated.
Neurofeedback training is a process by which an individual can change the way their brain operates. It is based on the premise that the human brain is plastic: it has the ability to alter its structure and function. During neurofeedback training, patients receive information about what their brain does naturally, and then they change it. How? By playing.
What would it mean—for humans and humanity—if play suddenly became purposeful?
We are all driven to play. We are motivated to solve the problems that keep us from winning games, completing puzzles, or scoring points. Yet, explaining this seemingly innate drive to play is difficult, as play is often characterized as an act performed without purpose and without the expectation of practical outcomes. It requires an appreciation of the means without a lust for the end. So, what would it mean—for humans and humanity—if play suddenly became . . . purposeful? Researchers are now harnessing this robust and universal motivation to play to treat patients suffering from psychiatric disorders. Let’s take a closer look at how this works.
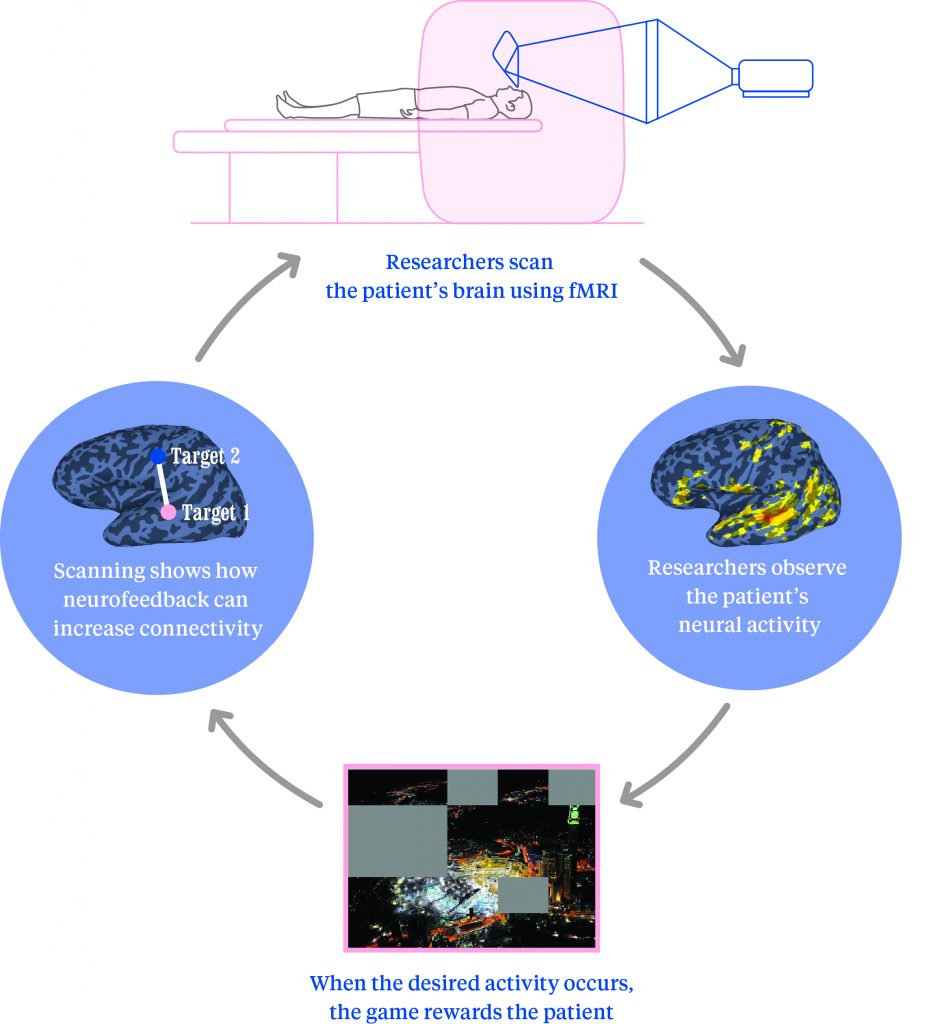
Many neurofeedback training programs employ a digital game interface to deliver feedback (from neuroimaging, for example) to patients about what their brains are doing: what parts of the brain are active, which regions are talking to which other regions, etc. When the desired regions of the brain spontaneously become active at the right time, patients receive a reward in the game, perhaps more points or an extra life. When patients’ brain activity fails to produce the desired pattern of neural activation, they do worse in the game. By repeating this protocol, patients with severe psychiatric illnesses can essentially change the activity patterns in their brain to function more like disease-free subjects, which in turn is associated with improved symptom severity.
Autism Spectrum Disorder (ASD) is a psychiatric condition characterized by difficulties in communicating and interacting in social settings. Neuroimaging studies have identified correlates of these behavioral symptoms at the level of neural connectivity: two key regions implicated in social processing, the superior temporal sulcus (STS) and the somatosensory cortex, have been shown to be connected more weakly—to “talk” to one another less—in ASD patients relative to healthy control subjects.
In a recent study published in the scientific journal eLIFE, researchers at the National Institute of Mental Health sought to ameliorate symptoms of ASD by increasing the connection between these two regions using neurofeedback training. fMRI neuroimaging was used to scan the brains of ASD patients (males fifteen to twenty-five years of age) while they played a video game. As part of the digital puzzle-like game, participants had to reveal regions of an image that were covered by a blank mask. They were not given any further instructions, but while they were playing the game, the fMRI scanner monitored the activity of the two brain regions of interest, the STS and the somatosensory cortex. When these two regions “talked” to one another (exhibiting the desired neural activity), patients were rewarded in the game: a piece of the masked image would become visible. Because the patients were motivated to play the game and uncover the masked images, over time, they learned to unconsciously reproduce the neural activity that resulted in this reward. And in the end . . . it worked!

Under some circumstances, our innate drive to play can be harnessed to heal.
By the end of the neurofeedback training regimen, ASD patients had significantly increased the connectivity between the STS and the somatosensory cortex even when they were no longer engaged in playing the video game (i.e. at rest). Importantly, this change in neural activity was correlated with a decrease in ASD symptom severity. Even more impressive, these changes in brain signaling were durable: they were still evident even a year after the neurofeedback training had ended. So, it appears that, under some circumstances, our innate drive to play can be harnessed to heal.
In response to this realization, I can’t help but wonder: what happens to our experience of play when it is endowed with purpose? Will our motivation to play dissipate the more utilitarian it becomes? Will the act of childhood play continue to promote healthy emotional development, as it has been shown to do in many species? At this point it may be too early to answer these questions. What is apparent, is that play holds the potential to help us learn, to help us grow, and now, to help us heal—at all ages of life. ♦